When the pandemic began two years ago, many policymakers and health officials worried over hospital capacity. Did hospitals — here and across the country — have enough beds to meet the expected flood of COVID-19 patients?
As the pandemic wore on, the concern shifted away from beds themselves and toward the doctors, nurses, respiratory therapists and other health providers who staff them. The pandemic’s politicization and relentless pace fueled burnout among America’s health care workforce, many of whom experienced verbal and physical harassment.

As many as one in five health care workers left the industry, according to one national survey. As a result, Colorado had hundreds fewer beds during the late 2021 surge than it had a year before.
Now, as the pandemic lulls, hospitals, nursing homes and the broader health system face a long road to recovery from the staffing shortages that predated COVID-19 and have significantly worsened since its arrival.
“What happened when the pandemic hit is there was a huge amount of burnout, and a huge amount of health care workers decided, ‘You know what? I’m over this,'” said Ramnik Dhaliwal, the president of the Colorado chapter of the American College of Emergency Physicians.
Colorado Board of Health extends health worker vaccine mandate, with eye toward permanent decision
Rebuilding the workforce is critical, added Eric Hill, emergency medical services director at the Medical Center of Aurora, particularly if the country saw another COVID-19 spike or a similar emergency.
“Right now, we’re doing OK,” Hill said of staffing. “But heaven forbid anything serious happens again because we’re not going to have the ability to surge again. Staffing hasn’t been replenished across the system yet.”

Holly Lawson, clinical coordinator at St. Francis Hospital, stands next to a new camera monitor system inside a room at St. Francis Hospital in Colorado Springs on Friday, March 25, 2022. Penrose- St. Francis is expanding the use of cameras that can monitor up to 10 patients at a time who might otherwise need a staff member in the room constantly. Hospitals, nursing homes and the broader health system face a long road to recovery from the staffing shortages. (Chancey Bush/ The Gazette)
Many hospitals have staffed up with newly graduated or traveling nurses to fill the positions vacated by those who’ve either retired, left the industry because of burnout, or switched to traveling roles for the significantly better paychecks. Physician shortages, a pre-pandemic problem fueled by limitations in physician training slots and an emphasis on subspecialty training, have also grown worse, as COVID-19 accelerated retirements and drove doctors out of the field.
While the number of hospitalized COVID-19 patients has dropped precipitously, down to eight in El Paso County, officials and providers have warned that the more standard patients they’re seeing now are sicker than they were pre-COVID because they delayed care. In some cases, the remaining staff are assigned more patients apiece than before.
The heavy workload has left staff feeling like they are not caring for patients as well as they could, contributing to burnout and morale concerns, said Laura Rosenthal, president of the Colorado Nurses Association.
When nurses have to take on the duties of other staff members, such as certified nursing assistants, who are typically responsible for tasks like bathing and feeding patients, that can further compound the problem, Rosenthal said.

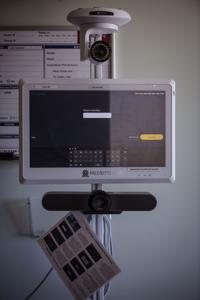
Debra Mireault, virtual telesitter, monitors patients using a new camera monitor system at St. Francis Hospital in Colorado Springs on Friday, March 25, 2022. Penrose- St. Francis is expanding the use of cameras that can monitor patients who might otherwise need a staff member in the room constantly. The cameras can monitor up to 10 patients. Hospitals, nursing homes and the broader health system face a long road to recovery from the staffing shortages. (Chancey Bush/ The Gazette)
Mark Johnson, the president of the Colorado Medical Society, added that nurses and health care workers generally are often saddled with heaps of administrative work, pulling them away from patient care and further fueling alienation.
The higher mix of new graduates and travelers into hospitals’ staffing is also not as safe as a robust, highly experienced, locally based staff, experts said. Many skills are universal, but travelers may not know hospital-specific protocols, around injury prevention or other initiatives.
“Would you rather have a nurse that has worked on that floor for a number of years,” Rosenthal asked, “or a nurse that just flew in from Texas?”
Some travelers are returning to full-time, locally-based jobs as COVID-19 ebbs nationally and demand for them dries up, said Rose Ann Scibona, chief nursing officer at Penrose Hospital. In the fall, Penrose-St. Francis had about 130 traveling nurses. That’s now halved, she said. It’s a helpful trend but not enough to address the broader problem.
Solving the staffing shortage will likely take a mix of efforts, such as higher pay, in-house training and incentive programs, a focus on wellness and employee buy-in, a strong graduate and training pipeline, and creative solutions involving new technology.

Penrose- St. Francis is expanding the use of cameras that can monitor up to 10 patients at a time who might otherwise need a staff member in the room constantly. Hospitals, nursing homes and the broader health system face a long road to recovery from the staffing shortages. (Chancey Bush/ The Gazette)
Penrose- St. Francis is expanding the use of cameras that can monitor patients who might otherwise need a staff member in the room constantly, Scibona said. A certified nursing assistant can watch about 10 patients at a time and send a staff member if a patient needs help but hasn’t called for it, like if they are pulling out their IVs or are unsteady on their feet. The cameras can also be set up for patients who need enhanced, but not constant, supervision.
The hospital is also mulling a similar program to allow an experienced intensive care unit nurse to monitor real-time patient health data on screens and alert other staff if they see a problem, she said.
Hiring new graduates is an obvious key to rebuilding the industry, but they are coming in at a challenging time, at higher proportions than pre-pandemic and leaving at higher numbers, officials said. Dhaliwal said throwing new graduates into high-intensity settings only sets them up for exhaustion and an early exit from medicine.
“I would say probably every emergency department in the state probably has multiple new grads,” he said, “when in the past, probably (hospitals) never would’ve allowed a new grad to come to the emergency department.”
At Penrose-St. Francis, an ICU- level nurse roves all the units helping to mentor and coach, assisting with reading lab results, X-rays and helping with patients, Scibona said. The hospital hired 60 to 70 new nursing graduates from the December graduating class; in all, the facility employs about 1,500 nurses.
Higher wages are key to the long-term solution, both to make up for what Dhaliwal described as a longstanding issue of underpaying nurses and to incentivize workers to stick around.
Johnson said traveling nurses could make multipliers above what their peers make, especially at the height of the pandemic. While the use of traveling agencies has slowed, their ability to command high dollar amounts and peal away workers showed the degree to which salaries needed to improve.
Glen Mays, the chair of the Department of Health Systems, Management & Policy at the Colorado School of Public Health, said salaries are key “if you want to get serious about addressing this chronic, long-term shortage of nurses.”
Compensation can be alleviated, he said, particularly if it’s viewed “as a priority for national preparedness.”
It’s an immediate-term fix, he continued, that can be accommodated by hospitals and health systems that “came through the pandemic pretty well,” financially speaking.
“They’ve got the profitability to spend in this area, given how important it is,” he continued.
Both Centura and UCHealth have bumped up pay and benefits in the wake of the pandemic.
Nurses and other health care workers also need to find meaning in their work and have access to wellness programs that are separated from human resources departments so that staff can feel like help is anonymous, Rosenthal said.
Hospital systems are working on better support for staff and wellness programs, said Darlene Tad-y, the vice president of clinical affairs for the Colorado Hospital Association.
In-house training and career advancement opportunities for nurses and other providers can also help retain staff, Dhaliwal and Mays said.
UCHealth’s recently launched in-house efforts to help staff start their health care career from scratch. For example, an employee could start out cleaning rooms without a high school diploma and UCHealth will fund their GED and additional education to move into a health care role, such as a phlebotomist, said David Steinbruner, chief medical officer for UCHealth Memorial Central and Memorial North.
But the staffing shortage issue is plagued further back, to the training and education pipelines for providers. There are too few residency slots for physicians, several officials said, to the point where some medical students in Colorado can’t make the next step in their training.
Johnson, of the state medical society, said medical education “is abysmal.” While residency programs are generally paid for via federal dollars, the state can do more to augment those funding levels.
“If we truly want to have well-trained health care workers, both in our major areas as well as rural and frontier areas, we have got to help support the training of people here in Colorado because people tend to stay where they train,” he said.
“We as a state have not done a good job of supporting the training. We have left it up to the programs. I think the legislature should be putting money into training programs in Colorado at a much higher rate than what we have done …, ” Johnson said.
“Individual states can also decide they want to invest proactively in opening residency slots,” Mays added. “It’s a matter of willingness to pay at a societal level, if the federal and state governments are willing to pay for extra residency slots.”
The high number of new graduates and travelers also makes it tough for nursing colleges to place students at facilities to gain necessary clinical experience, limiting the pipeline of new graduates for the industry and making it harder to recover from the staffing shortage, Rosenthal said. Many new graduates also did not receive the traditional in-person clinical training they would have during the pandemic because they were not allowed into hospitals.
Gary Winfield, the chief medical officer of HealthONE, said the aging physician and nurse workforce — and problems with physicians’ training programs — were “mega problems” before the pandemic; COVID-19 then accelerated retirements and departures.
Those losses have been particularly acute among primary care providers, said Larry Green, distinguished professor of family medicine at the University of Colorado, which will have ripple effects across the system. Good primary care treatment translates to healthier populations, lower costs and fewer inequities. He and others said medical training emphasized subspecialty training, meaning there are fewer generalists, which form the foundation of health care.
Hill, the Medical Center of Aurora physician, said people need to be “incentivized” to get into medicine, given the amount of time and money needed to enter the field. He and others ticked off grants, loan repayments and other financial incentives as ways to help remove barriers.
Across rural Colorado, hospitals have also been hit hard by the staffing shortages and in some cases nurses have left to work for nursing agencies only to end up working at the same facility making a lot more money, said Michelle Mills, CEO of the Colorado Rural Health Center.
The rates hospitals are paying traveling nurses are not sustainable, but there is not a clear solution to addressing the staffing issues in the short term, she said.
Lincoln Health Community Hospital in Hugo on the eastern plains is working on funding health science teachers at the local school district in the hopes some students can earn the qualifications to become a certified nursing assistants, she said. While much smaller in scale than UCHealth’s program, it aims to grow a local workforce in a similar way.
The state could provide some relief by funding local strategic health planning and for small rural hospitals to design their own solutions to the staffing shortages, she said.
“Grow-your-own programs are usually very successful for people,” she said, “because it has a lot of community buy-in.”
Dhaliwal agreed that rural facilities needed to be given a voice in how to address their own situation, and that their staffing struggles are both distinct and part of the broader issue facing the health system generally.
“One size does not fit all,” he said. “Allowing rural communities to decide which program is best for them or what mechanism is best for them might be the better way forward.”








More Stories
Top 5 Benefits of Seeing a Holistic Chiropractor
A New Smile, A New Life: The World of Dental Implantology
How to Get Rid of Type 1 Diabetes